Diagnostic Framework — The 2017 World Classification
Why revise the 1999 Armitage classification?
The Armitage (1999) classification distinguished "chronic" from "aggressive" periodontitis — two entities with major clinical overlap that made diagnosis imprecise. Experts at the 2017 World Workshop (AAP/EFP) concluded that the biological evidence did not support them as separate diseases. Periodontitis is now a single entity, structured along two independent dimensions: the Stage and the Grade.
This framework, inspired by oncology, enables treatment personalization based on current severity, management complexity and individual progression risk — a decisive advance toward precision periodontology.
Horizontal dimension — The Stage
- Determined by clinical attachment loss (CAL) at the most severe site
- Supplemented by radiographic bone loss and tooth losses
- Four stages: I (initial) → II (moderate) → III (severe) → IV (very severe)
- Stage is always assigned by the site of maximum destruction
Vertical dimension — The Grade
- Calculated from the bone loss-to-age ratio
- Modified by systemic risk factors
- Three grades: A (slow) → B (moderate) → C (rapid)
- Automatic upgrade to Grade C if smoking > 10 cig/day or HbA1c ≥ 7.0%
Staging — Severity and Management Complexity
Staging parameters — Reference table
| Parameter | Stage I | Stage II | Stage III | Stage IV |
|---|---|---|---|---|
| Interdental CAL | 1–2 mm | 3–4 mm | ≥ 5 mm | ≥ 5 mm |
| Bone loss | Coronal third (<15%) | Coronal third (15–33%) | Middle or apical third | Middle or apical third |
| Tooth loss | 0 | 0 | ≤ 4 teeth | ≥ 5 teeth |
| Probing depth (PPD) | ≤ 4 mm | ≤ 5 mm | ≥ 6 mm | Complex rehabilitation needs |
| Local complexity | Initial | Moderate | Class II/III furcation | Occlusal collapse, extreme mobility |
Grading — Progression Risk and Therapeutic Response
Grade criteria — Reference table
| Criterion | Grade A — Slow | Grade B — Moderate | Grade C — Rapid |
|---|---|---|---|
| Bone loss / Age ratio | < 0.25 | 0.25 to 1.0 | > 1.0 |
| Direct progression (5 years) | No evidence | < 2 mm | ≥ 2 mm |
| Modifier — Smoking | Non-smoker | < 10 cig/day | ≥ 10 cig/day |
| Modifier — Diabetes | Absent | HbA1c < 7.0% | HbA1c ≥ 7.0% |
S3 Protocol — Step 1: Biofilm Control and Risk Factor Management
Step 1 objectives
- Applies to all periodontal patients regardless of stage — mandatory prerequisite for subsequent steps
- Reduce the initial microbial load and create an environment favorable to healing
- Modify deleterious behaviors and systemic risk factors
- Secure active patient engagement before any subgingival instrumentation
Oral hygiene instruction (OHI)
- Mechanical toothbrushing (manual or powered): cornerstone of plaque control
- Interdental brushes: first choice when space permits — more effective than floss for reducing gingival inflammation at periodontal sites
- PMPR (Professional Mechanical Plaque Removal): supragingival scaling + removal of plaque retention factors
- Elimination of restoration overhangs and poorly contoured prosthetics
Risk factor management
- Smoking cessation: brief systematic counseling — tobacco impairs periodontal vascularity and immune response
- Diabetes: coordination with the medical team — target HbA1c < 7.0% to optimize periodontal stability
- Stress, obesity, xerostomic medications: identify and document
- Mandatory reassessment before progressing to Step 2
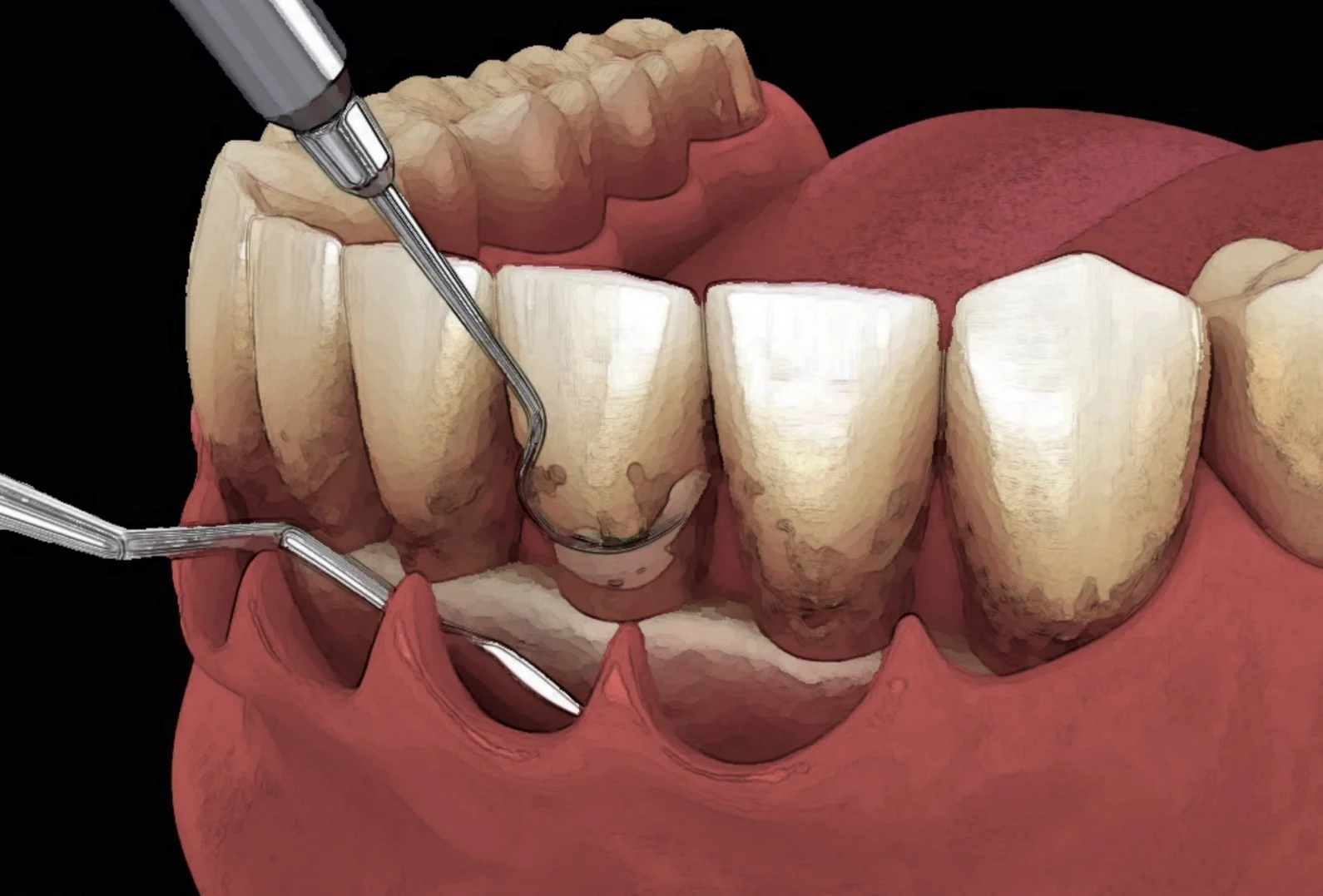
S3 Protocol — Step 2: Subgingival Instrumentation
Scaling and root planing (SRP) — Foundation of etiological treatment
Step 2 targets the elimination of subgingival biofilm and calculus to reduce probing pocket depth and promote pocket closure. Instrumentation may be performed with Gracey curettes (manual) or powered devices (ultrasonic/sonic), both showing similar clinical efficacy. The success criterion is pocket closure: PPD ≤ 4 mm with negative bleeding on probing (BOP).
Quadrant-by-quadrant instrumentation
- One quadrant treated at a time, at 1–2 week intervals
- Allows monitoring of tissue response between sessions
- Suited to patients with limited compliance
- Risk of bacterial recolonization of treated sites from untreated sites
Full-mouth disinfection (FMDis)
- Complete instrumentation in one or two closely spaced sessions (< 24 h)
- Often combined with chlorhexidine to limit recolonization
- Greater reductions in bleeding score (BS) and PPD vs quadrant approach
- FMDeb protocol (without antiseptic): comparable results, fewer constraints
S3 Protocol — Steps 3 and 4: Surgery and Maintenance
Step 3 — Surgical treatment of residual sites
Step 3 is indicated for sites that did not respond adequately to Step 2: persistent pockets ≥ 6 mm, or 4–5 mm pockets with persistent positive BOP. The choice of surgical technique depends on the morphology of the bony defect and the therapeutic objective (pocket reduction vs regeneration).
Surgical modalities — Comparative overview
| Surgery type | Primary objective | Indications | Key points |
|---|---|---|---|
| Open flap debridement (OFD) | Direct instrumentation | Deep pockets with difficult access | Limited pocket reduction |
| Resective surgery | Pocket elimination | Shallow bony defects, non-esthetic zones | Increased gingival recession |
| Regenerative surgery | Attachment restoration | Narrow intrabony defects, Class II furcations | Significant CAL gain |
Enamel matrix derivatives (EMD) or bone grafts with or without resorbable membranes are the materials of choice. Regeneration is recommended for mandibular molars and buccal maxillary Class II furcations.
Tunneling, root separation or root resection depending on morphology. These approaches require rigorous prosthetic planning and a tooth-by-tooth prognosis before proceeding.
Step 4 — Supportive Periodontal Care (SPC)
Maintenance is the most critical step for long-term stability. It begins as soon as periodontal health is achieved and must continue for life. Frequency is personalized using the Periodontal Risk Assessment (PRA).
High risk — Recall every 3 months
- Multiple sites with PPD ≥ 5 mm
- High BOP despite hygiene efforts
- Active smoking
- Poorly controlled diabetes (HbA1c ≥ 7%)
Low risk — Recall every 6–12 months
- Good plaque control (< 20%)
- Negative BOP on the majority of sites
- Non-smoker and well-controlled diabetes
- Radiographic stability at two successive check-ups
Adjunctive Therapies — Evidence and Recommendations
Amoxicillin + Metronidazole — Reference protocol
Amoxicillin (AMX)
Metronidazole (MET)
Expected results vs SRP alone: additional PPD reduction of 0.4–0.5 mm — CAL gain of 0.2–0.4 mm. Primary targets: Aggregatibacter actinomycetemcomitans and red complex bacteria.
Other adjuncts — Comparative evidence
Mouthwashes used as a temporary adjunct during post-instrumentation healing. Prolonged use limited by tooth staining and taste alterations.
Local delivery systems (CHX chips, metronidazole gel, minocycline microspheres): therapeutic concentration maintained in residual pockets ≥ 5 mm. Benefit is modest but statistically significant on PPD reduction.
aPDT (photosensitizer + low-level laser) reduces microbial load short-term, but meta-analyses show minor clinical benefits vs SRP alone — not recommended as a routine adjunct by S3 guidelines.
The LANAP protocol (Nd:YAG) selectively targets diseased tissue. Clinical studies: PPD and BOP reductions comparable or superior to SRP alone at one year, with better attachment stability.
Low-dose doxycycline (SDD) — 20 mg × 2/day: inhibits matrix metalloproteinases (MMPs) without selective bacterial pressure. Only FDA-approved systemic modulator. Not routinely recommended by EFP S3.
Natural products (curcumin, omega-3s, aloe vera): recent meta-analyses show significant improvement in PPD reduction and CAL gain as adjuncts — an interesting option requiring rigorous case selection.
Omega-3 fatty acids act as precursors of lipoxins and resolvins — pro-resolution mediators of chronic periodontal inflammation.
Of particular interest in Grade C patients resistant to instrumentation alone, as a complement to systemic risk factor control.
Stage IV — Multidisciplinary Management
The most complex clinical challenge
Stage IV combines periodontal support destruction with major functional and structural damage to the dentition. Rehabilitation requires a multidisciplinary team including a periodontist, orthodontist, prosthodontist and sometimes an oral and maxillofacial surgeon. The 2022 S3 guideline distinguishes four case types to structure management.
The four clinical case types of Stage IV
| Type | Clinical characteristics | Rehabilitation needs |
|---|---|---|
| Type 1 | Tooth loss without major migration | Standard periodontal treatment + maintenance |
| Type 2 | Pathological migration (diastemas, flaring) | Periodontal treatment + Orthodontics |
| Type 3 | Partial edentulism, reduced posterior support | Fixed or removable prostheses on teeth/implants |
| Type 4 | Complete or near-complete edentulism | Full-arch rehabilitation |
Mandatory treatment sequencing in Stage IV
Complete execution of Steps 1, 2 and 3 before any definitive prosthesis or orthodontic movement.
Teeth with a hopeless prognosis are extracted early to facilitate hygiene.
Provisional prostheses to stabilize the occlusion and assess patient cooperation.
Splinting of hypermobile teeth when necessary.
Correct migrations, close diastemas and restore occlusal relationships before definitive restoration.
Periodontal check-up every 3 months throughout active orthodontic treatment.
Natural tooth conservation must be prioritized over extraction for implant placement whenever biologically possible.
Confirmation of pocket closure, excellent oral hygiene and radiographic stability before any definitive impression.
Periodontitis and Systemic Health
Diabetes mellitus — Bidirectional relationship
- Uncontrolled diabetes increases the risk and severity of periodontitis
- Severe periodontitis can impair glycemic control
- SRP can produce an HbA1c reduction of approximately 0.4% — comparable to adding a second antidiabetic medication
- Shared goal with the treating physician: HbA1c < 7.0%
Pregnancy and maternal periodontitis
- Documented association with preterm birth, low birth weight and preeclampsia
- Periodontal treatment during pregnancy is safe and effective for improving maternal gingival health
- No systematic reduction in obstetric complications proven after SRP alone
- Treatment recommended in the 2nd trimester — priority on oral hygiene from the 1st trimester
Recent research suggests that oral pathobionts can migrate to the gut via the oral-gut axis, causing intestinal dysbiosis and exacerbating inflammatory conditions such as Crohn's disease, arterial hypertension and cardiovascular disease.
Periodontal treatment helps restore a healthier microbial profile both locally (gingival sulcus) and systemically (gut microbiome). An additional argument for early management of advanced stages.
Clinical FAQ
References
2017 Classification and diagnostic framework
-
1Guideline Papapanou PN, Sanz M, Buduneli N, et al. Periodontitis: Consensus report of workgroup 2 of the 2017 World Workshop on the Classification of Periodontal and Peri-Implant Diseases and Conditions. J Periodontol. 2018;89 Suppl 1:S173–S182.
efp.org — Consensus report workgroup 2, 2017 World Workshop -
2Review Mehta SB, Lim HC, Arora A, et al. Major highlights of the new 2017 classification of periodontal and peri-implant diseases and conditions. J Indian Soc Periodontol. 2021.
pmc.ncbi.nlm.nih.gov — Highlights of the 2017 classification -
3Review Buset SL, Walter C, Friedmann A, et al. Ease and practicability of the 2017 classification of periodontal diseases and conditions: a study of dental electronic health records. PMC. 2022.
pmc.ncbi.nlm.nih.gov — Ease and practicability of 2017 classification -
4Guideline Holtfreter B, Kocher T, Hertrampf K, et al. The 2018 EFP/AAP periodontitis case classification demonstrates high agreement with the 2012 CDC/AAP criteria. J Clin Periodontol. 2021.
ovid.com — 2018 EFP/AAP periodontitis case classification
EFP S3 guidelines — Treatment of Stages I to IV
-
5S3 Guideline Sanz M, Herrera D, Kebschull M, et al. Treatment of stage I–III periodontitis — The EFP S3 level clinical practice guideline. J Clin Periodontol. 2020;47 Suppl 22:4–60.
efp.org — S3-level guideline stages I–III (2020) -
6S3 Guideline Herrera D, Sanz M, Shapira L, et al. Treatment of stage IV periodontitis: The EFP S3 level clinical practice guideline. J Clin Periodontol. 2022;49 Suppl 24:4–71.
efp.org — S3-level guideline stage IV (2022) -
7Review Saleh MHA, Dias Rodrigues I, Shaddox L. Periodontitis: all change please? Introduction to the new S3-level treatment guidelines. JIDA. 2022.
jida.scholasticahq.com — Introduction to S3-level guidelines -
8Guideline EFP. STEP 4: Supportive periodontal care (SPC) — Guideline summary. European Federation of Periodontology, 2020.
efp.org — Step 4: Supportive periodontal care -
9Review Kebschull M, Papapanou PN. Diagnosis and Evidence-Based Treatment of Stage IV Periodontitis. Journal Agent PDF. 2022.
pdf.journalagent.com — Stage IV evidence-based treatment
Instrumentation and full-mouth debridement
-
10Clinical trial Eickholz P, Dannewitz B, Kimak A, et al. Management of periodontitis by three different approaches to non-surgical periodontal debridement — a randomized comparative clinical study. J Clin Periodontol. 2023.
pmc.ncbi.nlm.nih.gov — Three approaches to non-surgical debridement -
11Guideline ADA. Nonsurgical Treatment of Periodontitis Guideline. American Dental Association, 2023.
ada.org — Nonsurgical Treatment of Periodontitis Guideline -
12Guideline SDCEP. Supportive periodontal care — Prevention and Treatment of Periodontal Diseases in Primary Care. Scottish Dental Clinical Effectiveness Programme, 2022.
periodontalcare.sdcep.org.uk
Systemic adjunctive antibiotherapy
-
13Figuero E, Herrera D, Tobías A, et al. Efficacy of adjunctive systemic antimicrobials in periodontitis treatment: a systematic review and meta-analysis. J Clin Periodontol. 2014.
pmc.ncbi.nlm.nih.gov — Systemic antibiotic therapy in periodontics -
14Mistry A, Agrawal KS, Dhadse PV, et al. Amoxicillin/Metronidazole Dose Impact as an Adjunctive Therapy for Stage II–III Grade C Periodontitis at 3- and 6-Month Follow-Ups. EJOMR / PMC. 2024.
pmc.ncbi.nlm.nih.gov — AMX/MET dose impact meta-analysis -
15Nedzi-Gora M, Gorska R, Klosowska A, et al. The impact of systemic and topical antimicrobial therapy combined with non-surgical periodontal therapy: a meta-analysis. Advances in Clinical and Experimental Medicine. 2022.
advances.umw.edu.pl — Systemic and topical antimicrobial therapy -
16Review Levi I, Eini A, Kolerman R, et al. Targeted Use of Antimicrobials in Periodontal Therapy. Antibiotics / PMC. 2022.
pmc.ncbi.nlm.nih.gov — Targeted use of antimicrobials -
17Review EFP. Decision-making on systemic antibiotics in the management of periodontitis: a retrospective comparison of two concepts. European Federation of Periodontology.
efp.org — Decision-making on systemic antibiotics
Laser, aPDT and host modulation therapies
-
18Aljurbua A, Alqahtani S, Alafif T, et al. Efficacy of Antimicrobial Photodynamic Therapy for Treating Moderate to Deep Periodontal Pockets in Individuals with Type 2 Diabetes Mellitus: A Systematic Review and Meta-Analysis. MDPI / Antibiotics. 2024.
mdpi.com — aPDT and periodontal pockets in T2DM -
19Review Rajesh KS, Jacob R, Thomas B. Illuminating the path: the role of photodynamic therapy in comprehensive periodontal treatment. J Lasers Med Sci. 2024.
pubmed.ncbi.nlm.nih.gov — PDT in periodontal treatment -
20Clinical trial Nevins M, Kim SW, Camelo M, et al. Twelve-Month Follow-Up After the Treatment of Periodontal Conditions Using Scaling and Root Planning Alone vs. Laser-Assisted New Attachment Procedure. Int J Periodontics Restorative Dent. 2022.
pmc.ncbi.nlm.nih.gov — LANAP 12-month follow-up -
21Review Tuter G, Kurtis B, Serdar M. Host Modulation in Periodontology: Redefining Therapy Beyond Scaling and Root Planing. PMC. 2023.
pmc.ncbi.nlm.nih.gov — Host modulation in periodontology -
22Review Rosania AE, Low KG, McCormick CM, et al. Host modulation therapy in periodontitis, diagnosis and treatment — status update. Frontiers in Oral Health. 2023.
frontiersin.org — Host modulation therapy status update -
23Naqvi SH, Ahmed Z, Tanveer A. Do Adjunctive Therapies with Natural Products Improve Periodontal Outcomes? A Systematic Review and Meta-Analysis. MDPI. 2024.
mdpi.com — Natural products as adjunctive therapies
Oral microbiome, systemic interactions and maintenance
-
24Review Willis JR, Gabaldon T. Advancing periodontitis microbiome research: integrating design, analysis, and technology. Periodontol 2000. 2024.
pmc.ncbi.nlm.nih.gov — Periodontitis microbiome research -
25Longitudinal study Chen J, Chen Y, Hu L, et al. Correlation in the change of gut microbiota with clinical periodontal parameters in grade C periodontitis. PMC. 2024.
pmc.ncbi.nlm.nih.gov — Gut microbiota and grade C periodontitis -
26Longitudinal study Li Y, Zhao J, Zhang S, et al. Oral microbiome-based evaluation of periodontal treatment responses in individuals with special health care needs. J Oral Microbiol. 2023.
pmc.ncbi.nlm.nih.gov — Oral microbiome and periodontal treatment response -
27Tool Persson GR, Mancl LA, Martin J, et al. Periodontal Risk Assessment (PRA). perio-tools.com — Patient data-based periodontal risk calculator.
perio-tools.com — Periodontal Risk Assessment -
28Guideline ADA. Periodontitis — Clinical overview and management guidance. American Dental Association, 2023.
ada.org — Periodontitis overview -
29Guideline EFP. EFP Guideline: Treatment of periodontitis — Summary for clinicians. periodiabetes.org / EFP, 2020.
periodiabetes.org — EFP Guideline treatment of periodontitis